August 1, 2010 (Vol. 30, No. 14)
Carol Potera
Technology from Albert Einstein Medical School Being Developed by Makefield Therapeutics
Antibiotic-resistant strains of bacteria that cause superficial and invasive skin infections are on the rise. Among the victims are troops injured in Iraq and Afghanistan whose wounds become infected with microbes that are no longer killed reliably by methicillin and vancomycin.
Robert Towarnicki started Makefield Therapeutics in July 2009 to find novel treatments for antibiotic-resistant infections. The company, based in New Hope, PA, licensed a platform called Hybrid Nanoparticle™ technology that was discovered in Joel Friedman’s laboratory at the Albert Einstein College of Medicine in New York.
The Hybrid Nanoparticle technology delivers nitric oxide (NO) locally in a controlled and sustained manner. The platform is initially being evaluated as a topical treatment for skin infections and erectile dysfunction (ED). Peptides, nucleic acids, and traditional small molecule drugs can also be incorporated into the Hybrid Nanoparticle technology for oral, transdermal, intravenous, and intraperitoneal delivery.
The platform employs a biodegradable hydrogel made from ingredients on the FDA’s generally recognized safe list and/or the USP National Formulary. The hydrogel contains silane nanoparticles that release NO over time. A reaction between sodium nitrite and a sugar generates NO during the manufacturing process. The concentration of NO released and the time required is controlled by altering the amount and molecular weight of other ingredients such as polyethylene glycol or the concentration of encapsulated nitrite.
Chitosan is added to the NO nanoparticles to increase the antimicrobial killing action. This natural polymer, obtained from crustacean exoskeletons, binds to and disrupts the cell walls of bacteria. All the components of the nanoparticle delivery system are commercially available. The preparation methods use well-known pharmaceutical processes that easily lend themselves to scale-up and manufacturing.
NO shows broad-spectrum antimicrobial activity. In fact, Makefield researchers have not found any clinically relevant bacteria that are not killed by NO nanoparticles. However, the short half-life of NO makes it difficult to apply in the clinic.
“The challenge has been delivery,” says Towarnicki, president and CEO. “Our nanoparticles can be delivered transdermally and move through the skin into tissues, or they can be injected.”
Makefield will focus on the translational development of the NO-nanoparticle technology. Towarnicki hopes to file the company’s first IND application in 2011, which likely will cover a topical antimicrobial application.
Friedman’s laboratory has published several in vivo and proof-of-concept results across a variety of indications. Among the models is a murine wound model for methicillin resistant Staphylococcus aureus (MRSA) infections. Topically delivered NO nanoparticles increased wound healing, reduced bacterial burden, decreased inflammation, and prevented collagen degradation.
Similar results were shown in an animal model for wound infections caused by MRSA-resistant strains of Acinetobacter baumanni, a pathogen associated with battlefield injuries, surgical wounds, and ulcers. Mice receiving a single topical dose of NO nanoparticles healed more rapidly compared to untreated mice.
Another study of abscesses in mice infected with methicillin-resistant S. aureus found that topical or intradermal treatment with NO nanoparticles reduced the size of abscesses, bacterial load, and levels of pro-inflammatory cytokines, while improving skin architecture.
Based on these preclinical results, Makefield Therapeutics is optimizing formulations and picking lead indications. “Right now we’re leaning toward complicated skin and soft tissue infections where we can intervene and see immediate results,” says Towarnicki.
NO nanoparticles are not intended to replace oral or IV antibiotics but rather act as an initial therapy to control infections while physicians await the results of bacterial cultures to select the best antibiotic. The anti-inflammatory and antibacterial benefits of NO nanoparticles also lend themselves to a topical treatment for acne to avoid the systemic side effects of oral acne drugs. Additionally, the nanoparticles penetrate fingernails and toenails, making them a possible treatment for stubborn fungal infections.
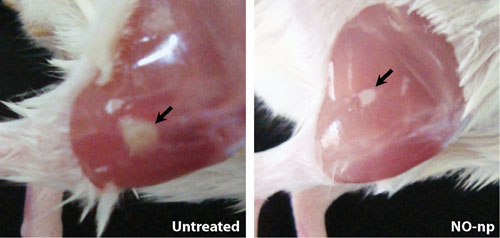
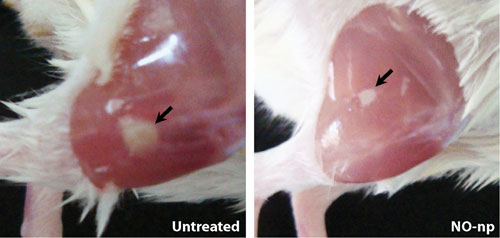
Nitric oxide nanoparticles (NO-np) decrease intramuscular abscess area in mice. Animals were inoculated intramuscularly in each flank (two abscesses) with 107 methicillin-resistant Staphylococcus aureus (MRSA), and 5 mg of lyophilized NO-np was topically applied per abscess, one and three days after infection. Abscess area analysis of Balb/c mice intramuscular lesions treated with NO-np (~1 mm2) is significantly smaller than untreated mice (~6.25 mm2). Arrows denote purulent abscess 4 days after MRSA infection.
Alternative for ED
NO is a potent vasodilator, too, making NO nanoparticles an ideal way to treat erectile dysfunction (ED). Despite widespread use of oral phosphodiesterase type 5 (PDE5) inhibitor drugs for ED, they have several drawbacks such as flushing, headache, and congestion. Moreover, patients with diabetes and other diseases often do not respond to oral PDE5 drugs. A topical treatment could overcome side effects and serve more types of men. “There’s a significant unmet need for better ED drugs,” says Towarnicki.
The nanoparticles can deliver current small molecule ED drugs as well as NO, as reported in January in the Journal of Sexual Medicine.
Topical treatment with nanoparticles encapsulating either NO or tadalafil (Cialis®) produced visible erections in a rat model for ED. There was no evidence of congestion or other side effects. And when oral doses of PDE5 inhibitors are compared to topical delivery in the nanoparticles, the topical formulations perform better, Towarnicki said.
Severed nerves, a consequence of prostatectomy, also cause ED. To simulate this condition, Makefield researchers severed the nerves of healthy young male rats. One week later, a topical dose of NO-nanoparticles spread on the rat penises caused erections.
“These are the exact nanoparticles that are antimicrobial, too,” Towarnicki points out. Different clinical needs can be met by optimizing the release kinetics of the nanoparticles. For instance, an antimicrobial can be designed to release NO for 24 hours at the site of an infection, whereas a treatment for ED would have a higher initial release rate followed by faster depletion.
Makefield Therapeutics plans to advance its therapeutics based on NO nanoparticles through Phase II trials. They will then look for partners for larger clinical trials and marketing.